Health systems across the world are evolving. However, the pace and focus of that evolution is a key determiner whether millions live longer, healthier lives or continue to bear the brunt of illness, disability and economic hardship. In an earlier piece, we discussed a strong economic case for preventive healthcare and the importance of centering healthcare systems around real people and real stories. This seems apparent in that, the future of health is not waiting for people to become sick and then treating disease. It is about preventing illness before it starts.
This shift from reactive to preventive healthcare is not only more humane; it is more cost-efficient and more sustainable, especially for countries like Nigeria and the broader African continent.
Preventive Healthcare Vs Reactive Healthcare
Preventive healthcare focuses on early detection and intervention to stop diseases from developing or progressing. Common preventive measures include vaccinations, routine health screenings, lifestyle counselling, health education, and regular medical check-ups. Evidence from multiple settings shows that when people engage in preventive care, serious health problems are either prevented or caught early when they are easier and cheaper to treat.
In contrast, reactive healthcare waits until symptoms become severe, often resulting in more complex treatments, higher costs, and poorer outcomes. This reactive model dominates much of healthcare in Nigeria and across Africa today, yet the burden of chronic and preventable disease is increasing rapidly.
The Growing Burden of Disease in Africa
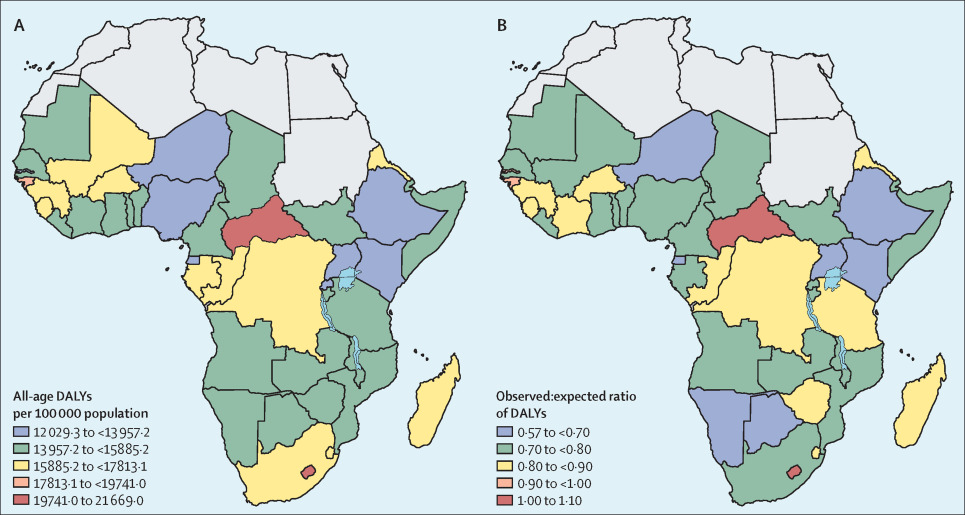
According to a February 2025 report by The Guardian, Africa’s medical system is set to collapse in just a couple of years with non-communicable diseases (NCDs) such as hypertension, diabetes, and cancer rising across Sub-Saharan African Regions. The report projects that these NCDs will become the leading causes of death by 2030. In 2019, NCDs already accounted for an estimated 37 percent of deaths in the region, up from 24 percent in 2000. Hospitals also report that up to half of admissions are now related to NCDs, these are conditions that could often be prevented or mitigated with effective early detection and lifestyle care.
This shifting disease profile makes clear that investment in preventive health is not a luxury, it is a necessity if health systems are to remain functional and resilient.
However, In Nigeria, Africa’s largest nation by population, many people still seek medical care only when illness becomes severe! Studies show that fewer than 40 percent of Nigerians visit health facilities for routine or preventive check-ups when they are not seriously ill, even though awareness of preventive care is high. Cost, distance to services, and low health insurance coverage are other major barriers.
Another survey in an Abuja private hospital found that while over 90 percent of patients understood the value of preventive care, only a minority actually utilised services unless symptoms were present. High healthcare costs, lack of insurance and logistical barriers were repeatedly cited.
Other evidence confirms that preventive services are under-utilised in rural communities, with fewer than half of older adults accessing basic preventive care.
Signs of Progress in Preventive Healthcare
Nigeria has already demonstrated that preventive approaches can work at scale. The national vaccination drive against human papillomavirus (HPV) reached over 12 million girls and is a key strategy to prevent cervical cancer, illustrating how organised preventive programmes can produce measurable outcomes.
Attached to government efforts are private facilities like Purelife Health which is specifically targeted at reducing the burden of reactive healthcare by providing essential primary healthcare services, quality medication and access to health education to every day Nigerians.
Digital health technologies are also emerging as powerful tools to amplify preventive health efforts. Mobile applications, telemedicine platforms and data analytics can help track health trends, deliver reminders for screenings, and bring healthcare services to underserved communities. These innovations make preventive health more accessible and personalised, particularly in areas with limited physical infrastructure.
For Nigeria and Africa at large, embracing preventive health is not optional as it is very essential for sustainable development. As the disease landscape evolves, health systems must pivot toward early detection and risk mitigation. Such a shift will reduce mortality and morbidity from chronic diseases, lower healthcare costs for families and governments, improve quality of life and workforce productivity and strengthen health system resilience in the face of both chronic and emerging threats.

Leave a comment